MESENCHYMAL STEM CELLS: Evaluating its regenerative potential in COVID-19
Severe acute respiratory syndrome coronavirus 2 (SARS-CoV- 2) is a highly contagious virus that caused the COVID-19 disease. After the first cases were reported, it rapidly disseminated across the world in a short period of time, proving to be the most serious and life-changing health crisis since the deadly influenza pandemic in 1918. The World Health Organization (WHO) was impelled to declare the COVID-19 disease as a global pandemic outbreak, which had led to the exhaustion of healthcare systems following the uncontrollable spread within months of its and eventually resulted in the loss of livelihoods due to the continued lockdown
During the onset of the pandemic, there were many crucial questions circulating large number of infected people, it is presumed that this pathogen has a zoonotic around the disease and its source. Based on the detailed investigations on the origin. The symptoms of infection normally appear after an incubation period of 5 to 6 days. But the time a person gets infected, symptoms to possible death ranged from 6 to 41 days with a median of 14 days. This period is dependent on the age and status of the patient’s immune system.
In addition, as the disease displays a wide spectrum of clinical presentations that range from asymptomatic infection to death-threatening cases, the WHO has estimated that the average fatality rate for COVID-19 is 2.2%. Higher mortality risk factors include a number of factors: age over 60 years, obesity, male gender, smoking, and presence of preexisting conditions such as cardiovascular and chronic pulmonary diseases, diabetes, cancer, solid organ or hematopoietic stem cell transplant. The hospitalization rate was six times higher as well in patients who have some of the above mentioned risk factors (45.4% of patients with reported underlying comorbidity vs. 7.6% of patients without reported underlying comorbidity).
From the million individuals who have been infected, most common symptoms of COVID-19 disease are fever, cough, fatigue, headache, haemoptysis, diarrhoea, and dyspnea. Due to this virus primarily targeting the human respiratory system, clinical features revealed by a chest CT scan could be presented as pneumonia and ground-glass opacities in subpleural regions of both lungs. These opacities are the result from both systemic and localized immune response, and showed increased inflammation process. Blood tests of COVID-19 patients, on the other hand, show lymphopenia (47.6%) with an increased amount of neutrophils. This elevated neutrophil-to-lymphocyte ratio (NLR) points to the onset of cytokine- induced inflammatory storm and appeared to be a sensitive predictor of disease severity. Other laboratory tests could show elevated C-reactive protein levels (65.9%), elevated cardiac enzymes (49.4%), abnormal liver function tests (26.4%), elevated D-dimer (20.4%), elevated erythrocyte sedimentation rate (20.4%), leukocytosis (9.9%), upregulated procalcitonin (16.7%), and abnormal renal function (10.9%).
In these circumstances, the common SARS-CoV-2 transmission is through respiratory droplets containing the virus while in close contact with individuals with COVID-19. That is why, the use of a standard three-layer surgical mask in public places could significantly reduce the risk of disease compared to a simple cloth mask that does not provide adequate isolation from the virus particles and gives a false sense of protection. The virus was also found to be stable on stainless steel and plastic for up to 2 to 3 days, which is why individuals can be easily infected via contact with surfaces contaminated with the virus. As a result, thorough hand sanitation or decontamination of product packages from a store by using disinfectants (such as 70% alcohol solution) will help reduce the risk of illness. Similarly, SARS-CoV-2 live virus particles are found in feces of infected people, indicating a possible fecal-oral transmission. Thus, proper hygiene and keeping distance from others can also lower the risk of getting infected.
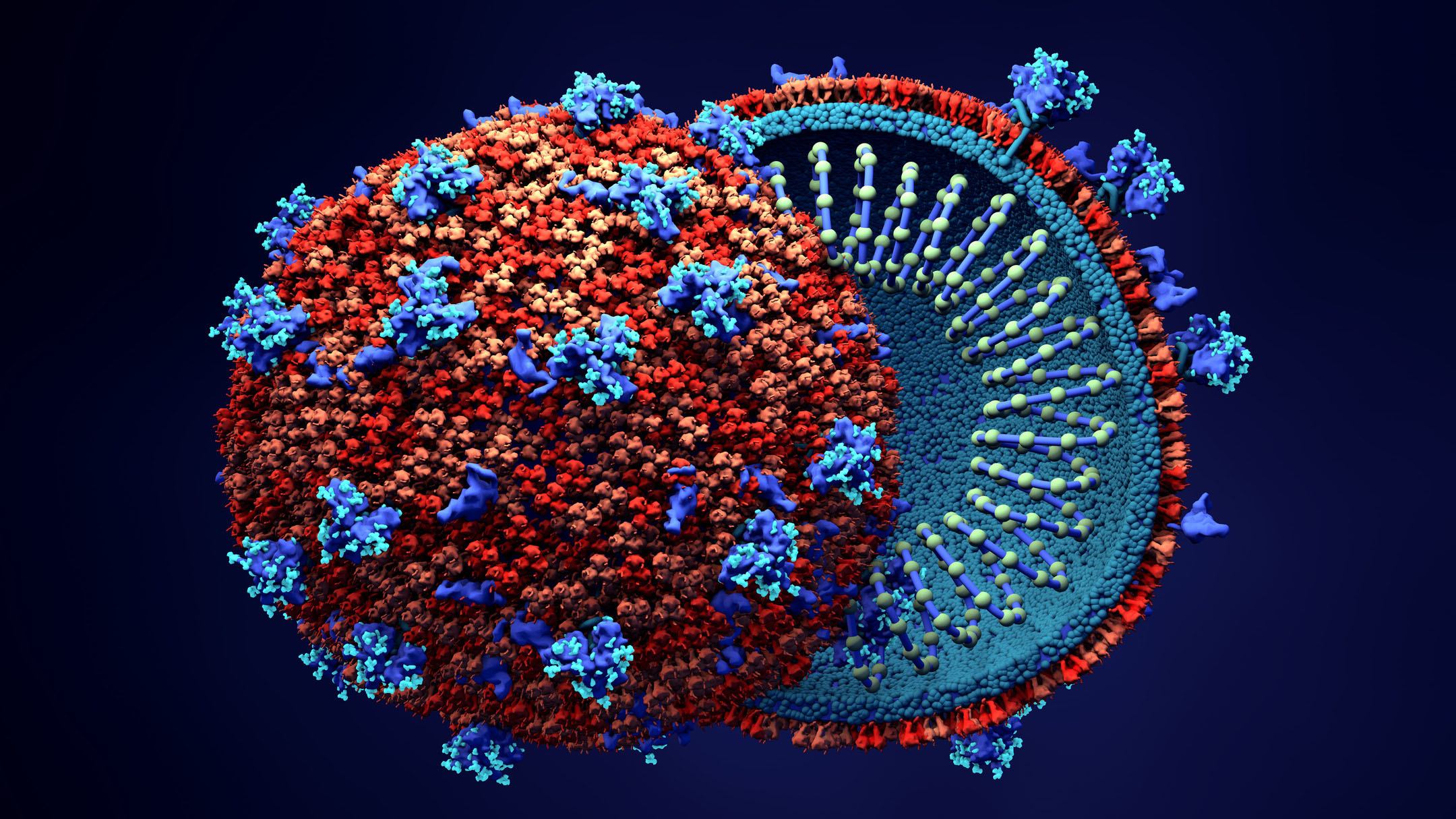
Thus far, a number of vaccines have been developed to significantly reduce the risk of the COVID-19. This means, getting vaccinated is recommended to everyone, particularly those with contraindications to immunization. It is known that SARS-CoV-2 enters the host cells after virus spike protein (or S protein) bind to the cellular receptor of angiotensin-converting enzyme 2 (ACE2). The immune response (antibodies and T-cells) during vaccination is formed to recognize this S protein. When the virus particles enter the vaccinated person's body, antibodies bind to the S protein and block its interaction with the ACE2 receptor, thereby, preventing the replication of the virus and the development of the disease. Although some emerging variants of concern have changes in the structure of the S protein and may be more virulent than the original strain, it has been shown that a booster shot of vaccine six months after initial vaccination induces a more mature and stable immune response, which provides an increased protection against SARS-CoV-2 virus, including novel variants (delta and delta+).
That being said, the clinical presentation and development of COVID-19 disease ranging from minor common cold symptoms to severe acute states were found to affect not only the respiratory system but also many other organ systems (renal, cardiovascular, gastrointestinal, cerebrovascular, or hepatobiliary).
Thus, the development of COVID- 19 disease can be roughly divided into two phases. The early phase is characterized by the onset of symptoms. This is when SARS-CoV- 2 virus is actively replicating and could directly harm ACE2-positive tissues.
The later phase, on the other hand, is accompanied by hyperinflammation and prothrombotic condition. This is when SARS-CoV-2 virus is practically absent, but the immune cells, such as T lymphocytes and monocytes are releasing cytokines that could seriously damage healthy tissues. In severe COVID-19 cases, the immune system's overactivation results in a 'cytokine storm' characterized by the release of huge amounts of cytokines (IL-6, TNF-α, IL-8, MCP1, RANTES) into the blood, causing multiple organ dysregulation and eventually death. In this regard, intense efforts of clinical researchers across the world has resulted in the development of several therapeutic options for the COVID-19 treatment, depending on the severity of the illness, the stage of the disease, and presence of certain mortality risk factors.
The variety of therapeutic options that are currently available include antiviral medications (e.g. remdesivir) and anti-SARS-CoV-2 monoclonal antibodies ( BLAZE-1 or bamlanivimab/etesevimab, REGN-COV2 or casirivimab/imdevimab) that are applicable during the early phase of the disease for reducing viral load. Anti-inflammatory drugs such as corticosteroids (e.g. dexamethasone), and immunomodulating agents (e.g. baricitinib, tocilizumab) will help to control hyperinflammation in the later phase and prevent multiple organ damages. Low weight heparins and other anticoagulant drugs are prescribed to prevent tromboembolia and possible complications associated with it (myocardial infarction, stroke, deep venous thromboembolism, etc.).
To date, there is a great effort from the scientific community to further seek other novel therapies capable of reaching multiple organs affected by COVID-19. Therapy with mesenchymal stem cells (MSC) shows good results in regenerative and transplant medicine to prevent graft-versus-host disease (GVHD). MSCs have immune modulating, immunosuppressive, antifibrotic, and anti-apoptotic effects. In the case of COVID-19, MSCs, due to their immunomodulatory activity, can help to prevent a cytokine storm and therefore reduce the likelihood of a severe course of the disease and the development of serious complications. MSCs produce prostaglandin E2 and can promote polarization of macrophages from M1 to M2 anti-inflammatory phenotype, increasing production of anti- inflammatory cytokine IL-10. Likewise, it was suggested that the direct lesion of endothelial cells could play a central role in the onset of COVID-19 coagulopathy and thrombotic disorder. From this perspective, the anti-apoptotic activity of MSC promotes the preservation of endothelial cells of the lung alveoli and blood vessels, thereby reducing tissue damage and the risk of thrombosis, as well as improving lung function. MSCs secrete vascular endothelial growth factor (VEGF) and hepatocyte growth factor (HGF), contributing to endothelial barrier stabilization in pulmonary capillaries, inhibition of endothelial cell apoptosis, and vascular endothelial (VE)-cadherin recovery. Additionally, it was revealed that MSCs do not possess ACE2 receptors and therefore could not be infected by SARS-CoV-2 virus. This fact ensures that MSCs could not be infected and destroyed by virus, which means all their therapeutic activities after injection to the SARS-CoV-2 infected patient are retained.
While MSCs have emerged as potential instruments in therapy due to the observed therapeutic mechanisms, there are no approved MSC-based strategies yet for the prevention or treatment of COVID-19 patients. In addition, the use of dexamethasone to decrease inflammation process has a negative effect on MSCs, thereby reducing their therapeutic efficacy. As such, MSC has a narrow therapeutic window when used before a patient undergoes a hormone treatment. We believe that MSC therapy is of high demand in the recovery period after a disease.
On a different note, pulmonary fibrosis is a typical complication of SARS-CoV-2 infection. MSCs could help in improving pulmonary function and regenerate the lungs due to their anti-fibrotic activity. MSCs are also able to improve the condition of patients with complications on the kidney, heart, and brain through their immunomodulatory antiapoptotic and antifibrotic paracrine mechanisms. Besides the paracrine effect, it was shown that mitochondrial transfer also plays a role in the regeneration and repair of organs. The mitochondrial transfer from bone marrow-derived MSCs in particular, was found to have the ability to regulate levels of Bcl-2, Bax, and PGC-1α, and inhibit reactive oxygen species (ROS) production, thereby suppressing apoptosis of cells.
In such event, Kintaro cells are bone marrow derived mesenchymal stem cells that have great regenerative capacities and possess very promising regenerative therapeutic potential for patients suffering COVID-19 disease. After intravenous administration, Kintaro cells easily accumulate in the lungs and minimize the negative effects of COVID-19, thereby restoring the damaged organ systems and reviving them to normal functioning. Therapy with Kintaro cells could be started two days after termination of dexamethasone (or other steroid anti-inflammatory drug) intake. Kintaro cells therapy might be also tried during COVID-19 disease if there is an increased risk of developing a cytokine storm.

Sources:
- https://www.ncbi.nlm.nih.gov/books/NBK554776/
- https://www.nature.com/articles/s41536-021-00147-x
- https://journals.sagepub.com/doi/full/10.1177/0885066621997365
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8049196/
